Welcome to the Ultimate Mole Removal Resource
If there’s one thing we know at Moles.org, it’s moles. Yes, our domain name is literally Moles.org—we’re THAT committed to being your go-to resource for everything mole-related. While we cover chemistry moles, yard moles, and skin moles, this particular guide is dedicated entirely to removing the skin variety.
We’ve put together the most comprehensive mole removal guide on the internet because we believe you deserve clear, accurate, and yes, entertaining information about your options. Whether you’re researching for medical reasons, cosmetic concerns, or just intense curiosity, you’re in the right place.
What makes us the mole experts? Our name says it all. At Moles.org, moles are literally our thing. We’ve researched every method, talked to dermatologists, reviewed the studies, and compiled everything into one massive guide so you don’t have to spend hours Googling at 2 AM.
Let’s dive into everything you need to know about mole removal—from professional procedures to what NOT to try at home.
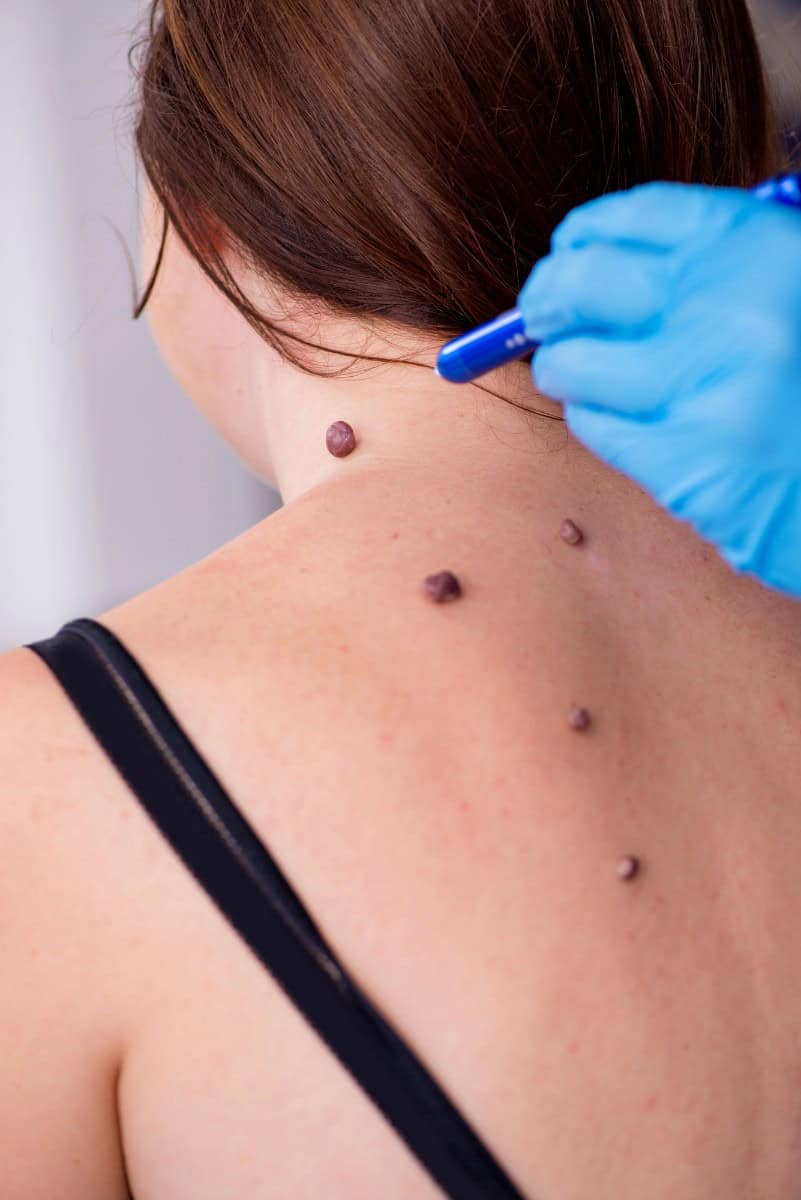
Table of Contents: Your Mole Removal Roadmap
Quick Navigation:
- What Is Mole Removal?
- When Should You Remove a Mole?
- All Mole Removal Methods Explained
- Mole Removal Cost Guide
- Healing Stages & Timeline
- Scarring: What to Expect
- Minimizing Scars: Battle Plan
- Insurance Coverage
- Aftercare Instructions
- DIY Mole Removal: Just Don’t
- Special Cases & Locations
- Recovery: What to Really Expect
- When Moles Come Back
- What to Ask at Your Consultation
- Provider Red Flags
- Kids, Pregnancy & Seniors
- New Technology & What Works
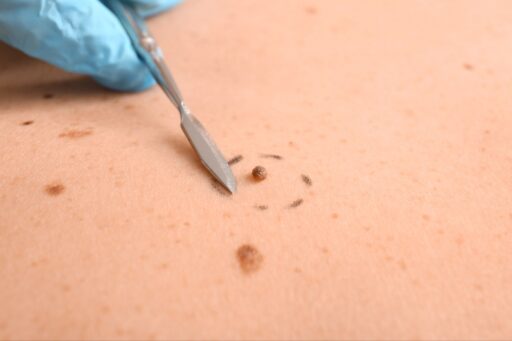
What Is Mole Removal? The Basics
Mole removal is exactly what it sounds like: a medical procedure to remove a mole (nevus) from your skin. But it’s not quite as simple as just “taking it off.”
The procedure can involve:
- Surgical excision (cutting it out with a scalpel)
- Shave removal (shaving it off at skin level)
- Laser treatment (using focused light energy)
- Cryotherapy (freezing with liquid nitrogen)
- Radiofrequency ablation (using radio waves)
The method used depends on the mole type, location, size, whether it’s suspicious, and whether you want it biopsied.
Why people get moles removed:
- Medical reasons: Suspicious or atypical moles that need biopsy
- Cosmetic reasons: Don’t like how it looks
- Practical reasons: Gets irritated by clothing, jewelry, or shaving
- Precautionary reasons: Family history of melanoma
Important distinction: Medical removal (suspicious moles) vs. cosmetic removal (benign moles you just don’t like) matters for insurance coverage, which we’ll get into later.
When Should You Remove a Mole?
Not every mole needs to come off, but here at Moles.org, we know certain situations absolutely warrant removal:
You SHOULD Get a Mole Removed If:
- It’s changing: Size, shape, color, or texture changes
- It follows the ABCDEs:
- A – Asymmetry (one half doesn’t match the other)
- B – Border irregularity (jagged, notched, or blurred edges)
- C – Color variation (multiple colors, uneven color)
- D – Diameter (larger than 6mm/pencil eraser)
- E – Evolving (changing over time)
- It bleeds or itches: Spontaneous bleeding or persistent itching
- Dermatologist recommends it: They’re the experts, listen to them
- It’s atypical/dysplastic: Biopsy showed abnormal cells
- Family history: You have melanoma in your family
You MIGHT Want to Remove a Mole If:
- It bothers you cosmetically
- It gets irritated by clothing or jewelry
- You cut it while shaving
- It’s on your face and you don’t like it
- It catches on things
You Probably DON’T Need to Remove a Mole If:
- It’s small, stable, and not changing
- Your dermatologist says it’s fine
- It’s been there your whole life without issues
- It doesn’t bother you
The golden rule from the mole experts: When in doubt, see a dermatologist. We may be Moles.org, but we’re not replacing professional medical advice!
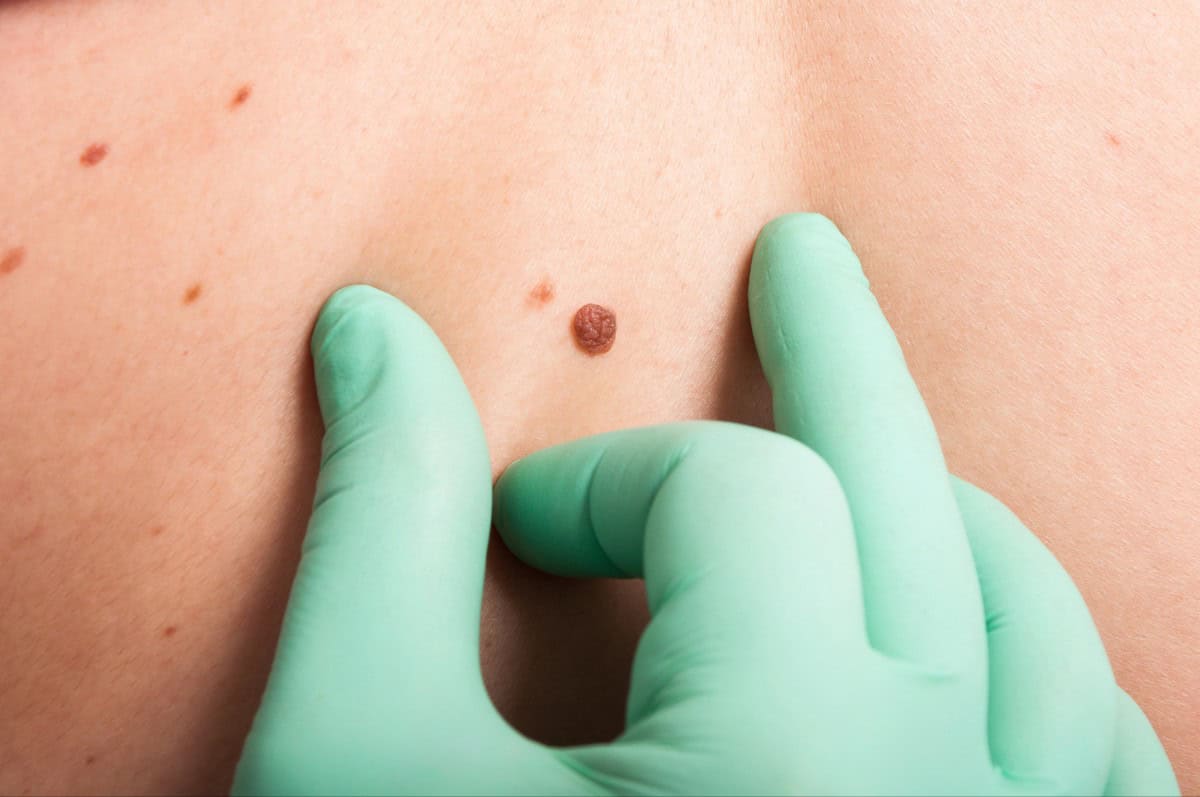
All Mole Removal Methods Explained
Here’s where we get into the good stuff. There are several ways to remove moles, and we’re covering ALL of them—the good, the bad, and the “please don’t try that.”
1. Surgical Excision (The Gold Standard)
What it is: The dermatologist cuts out the entire mole and some surrounding tissue, then stitches the wound closed.
Best for:
- Suspicious or atypical moles
- Deep moles
- Moles that need biopsy
- When you want lowest recurrence rate
The procedure:
- Local anesthetic injection (small pinch, then numb)
- Mole cut out with scalpel in elliptical shape
- Wound closed with stitches (internal and/or external)
- Tissue sent to lab for biopsy
- Stitches removed after 5-14 days (depending on location)
Pros:
- Complete removal—lowest chance of regrowth
- Tissue can be biopsied (cancer screening)
- Works on all mole types
- Predictable results
Cons:
- Requires stitches
- Linear scar (usually fades well)
- Longer healing time (2-3 weeks)
- Can’t get wet for several days
Recovery: 2-3 weeks for initial healing, several months for scar to fully mature
Cost: $150-$600 (more with insurance if medically necessary)
2. Shave Removal (The Quick Option)
What it is: The dermatologist uses a surgical blade to shave off the mole at skin level, then cauterizes the base.
Best for:
- Raised moles
- Benign moles (already confirmed non-cancerous)
- Cosmetic removal
- Moles that stick out from skin
The procedure:
- Local anesthetic
- Mole shaved off flush with skin
- Base cauterized to stop bleeding
- Bandage applied
- No stitches needed
Pros:
- Quick (5-10 minutes)
- No stitches
- Fast healing
- Less expensive than excision
Cons:
- Higher chance of mole growing back (roots may remain)
- Can’t biopsy as thoroughly
- Not suitable for suspicious moles
- May leave slight indentation or texture change
Recovery: 1-2 weeks
Cost: $100-$400
3. Laser Mole Removal (The High-Tech Option)
What it is: Focused laser energy breaks down mole cells, which are then absorbed by the body.
Best for:
- Small, flat, benign moles
- Facial moles (cosmetic concerns)
- Multiple small moles
- When minimal scarring is priority
Types of lasers used:
- CO2 laser (most common)
- Erbium laser
- Q-switched lasers
The procedure:
- Topical numbing cream or local anesthetic
- Laser pulses applied to mole
- Multiple sessions often needed
- No bleeding, no stitches
Pros:
- Minimal scarring potential
- No cutting or stitches
- Quick procedure
- Good for multiple small moles
Cons:
- Can’t biopsy tissue (it’s vaporized!)
- Only for clearly benign moles
- Often needs multiple sessions
- Risk of hypopigmentation (light spots)
- Not suitable for deep or suspicious moles
- Results vary widely by practitioner
Recovery: 1-2 weeks per session
Cost: $200-$500 per session (often need 2-3 sessions)
4. Cryotherapy (Freezing)
What it is: Liquid nitrogen applied to freeze and destroy mole tissue.
Best for:
- Honestly? Not ideal for moles at all
- Better for warts and other skin lesions
- Occasionally used for small, flat moles
The procedure:
- Liquid nitrogen applied with cotton swab or spray
- Area freezes and blisters
- Blister eventually falls off
- May need repeat treatments
Pros:
- Quick and inexpensive
- No cutting
Cons:
- Can’t biopsy tissue
- High risk of permanent light spots (hypopigmentation)
- Not effective for deep moles
- Often leaves noticeable mark
- Multiple treatments usually needed
The verdict from Moles.org: We generally don’t recommend cryotherapy for moles. It’s great for warts, but there are better options for moles.
Recovery: 1-3 weeks
Cost: $100-$300
5. Radiofrequency/Electrosurgery
What it is: High-frequency radio waves cut through tissue and simultaneously cauterize.
Best for:
- Small to medium raised moles
- Cosmetic removal
- Skin tags and similar lesions
The procedure:
- Local anesthetic
- Radiofrequency device removes mole layer by layer
- Simultaneous cutting and cauterizing
- No stitches typically needed
Pros:
- Precise control
- Less bleeding than traditional methods
- Can preserve tissue for biopsy (unlike laser)
- Faster healing than excision
Cons:
- Not as common—requires special equipment
- Learning curve for practitioners
- May need multiple passes
Recovery: 1-2 weeks
Cost: $200-$600
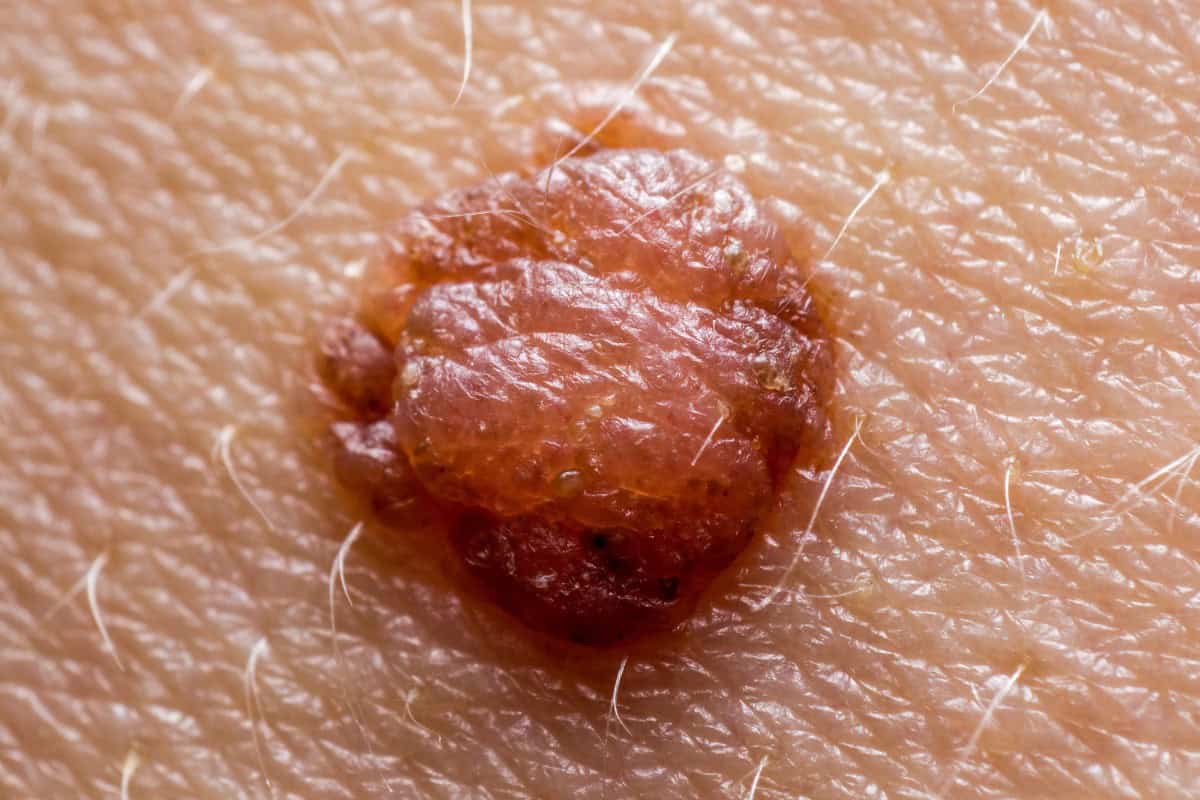
Mole Removal Cost: Breaking Down the Bill
Let’s talk money, honey. As the financial experts at Moles.org (okay, we’re mole experts, but we know the costs), here’s what you’re looking at:
Average Costs by Method:
Surgical Excision: $150-$400 per mole
- Hospital/surgical center: $500-$1,500
- With biopsy: Add $100-$300
- Multiple moles: Some discount usually
Shave Removal: $100-$300 per mole
- Quick office procedure
- Often bundled pricing for multiple moles
Laser Removal: $200-$500 per session
- May need 2-3 sessions
- Total cost: $400-$1,500
- Rarely covered by insurance
Cryotherapy: $100-$300
- Quick and cheap
- But remember: you get what you pay for
Dermabrasion/Radiofrequency: $200-$600
- Varies widely by provider
- Geographic location matters
Geographic Price Variations:
- New York City/Los Angeles/San Francisco: +50-100% above average
- Rural areas: 20-40% below average
- Medical tourism (Thailand/Mexico): 60-80% cheaper (proceed with caution)
What Affects the Cost:
- Location on body: Face costs more than trunk
- Mole size: Larger moles = higher cost
- Number of moles: Bulk discounts often available
- Complexity: Deep or difficult moles cost more
- Provider type: Dermatologist vs. plastic surgeon vs. general practitioner
- Facility: Office vs. surgical center vs. hospital
- Geographic area: Major cities cost more
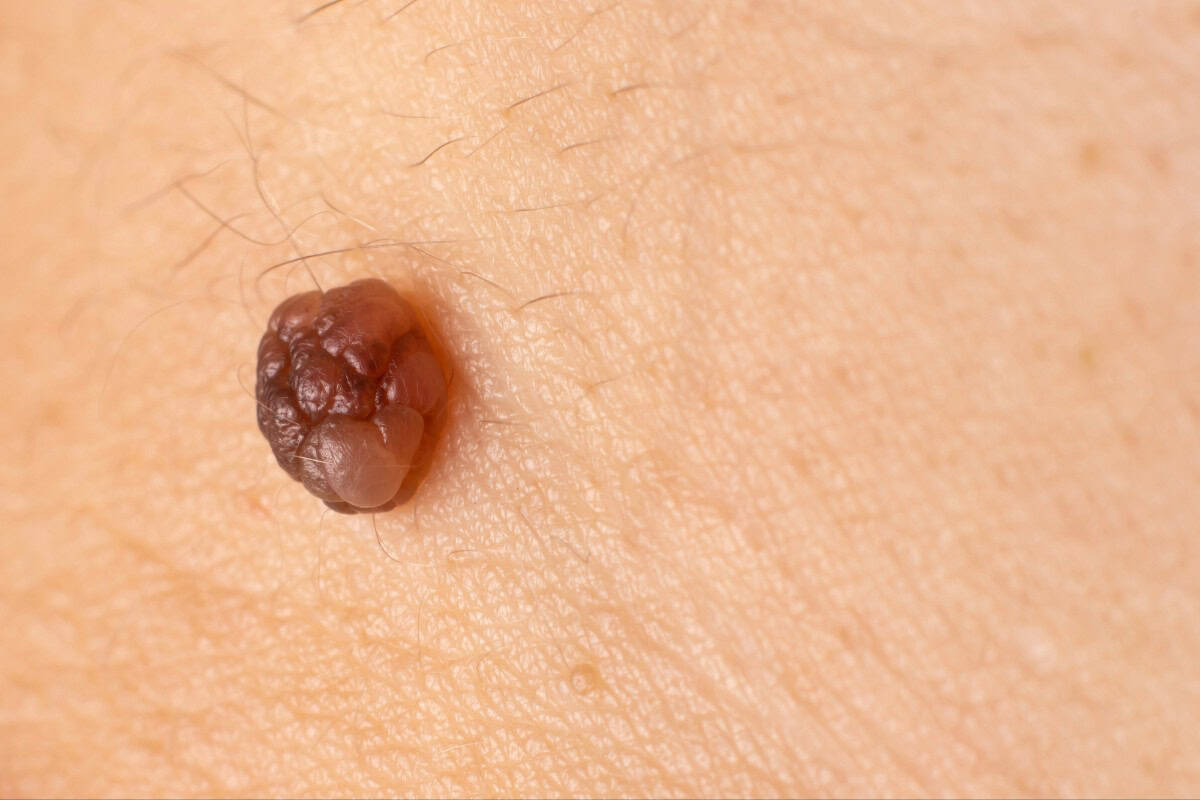
Insurance Coverage: The Great Mole Removal Lottery
When Insurance Usually Covers It:
- Suspicious/atypical moles (pre-cancerous)
- Melanoma concerns
- Moles causing physical problems (rubbing, bleeding, pain)
- Recent changes documented by physician
- Medical necessity documented in chart
When You’re Paying Out of Pocket:
- Purely cosmetic removal
- “I just don’t like how it looks”
- Preventive removal of normal moles
- Laser treatment (almost never covered)
- Multiple cosmetic moles at once
Insurance Approval Tips from the Moles.org Playbook:
- Document everything: Photos, descriptions of symptoms
- Magic words: “Changing,” “bleeding,” “painful,” “catching on clothing”
- Get pre-authorization: Don’t assume coverage
- Ask about medical necessity: Have your doc document it
- Appeal if denied: Many denials are overturned on appeal
- Know your deductible: Coverage doesn’t mean free
Typical Insurance Coverage Scenarios:
Best Case (Full Coverage):
- Dermatologist documents concerning features
- Biopsy shows dysplasia
- You’ve met your deductible
- Out of pocket: $0-$50 copay
Middle Ground:
- Some features concerning, some cosmetic
- Haven’t met deductible
- Out of pocket: $150-$500
Worst Case (No Coverage):
- Purely cosmetic
- You pay cash
- Out of pocket: $200-$1,500+
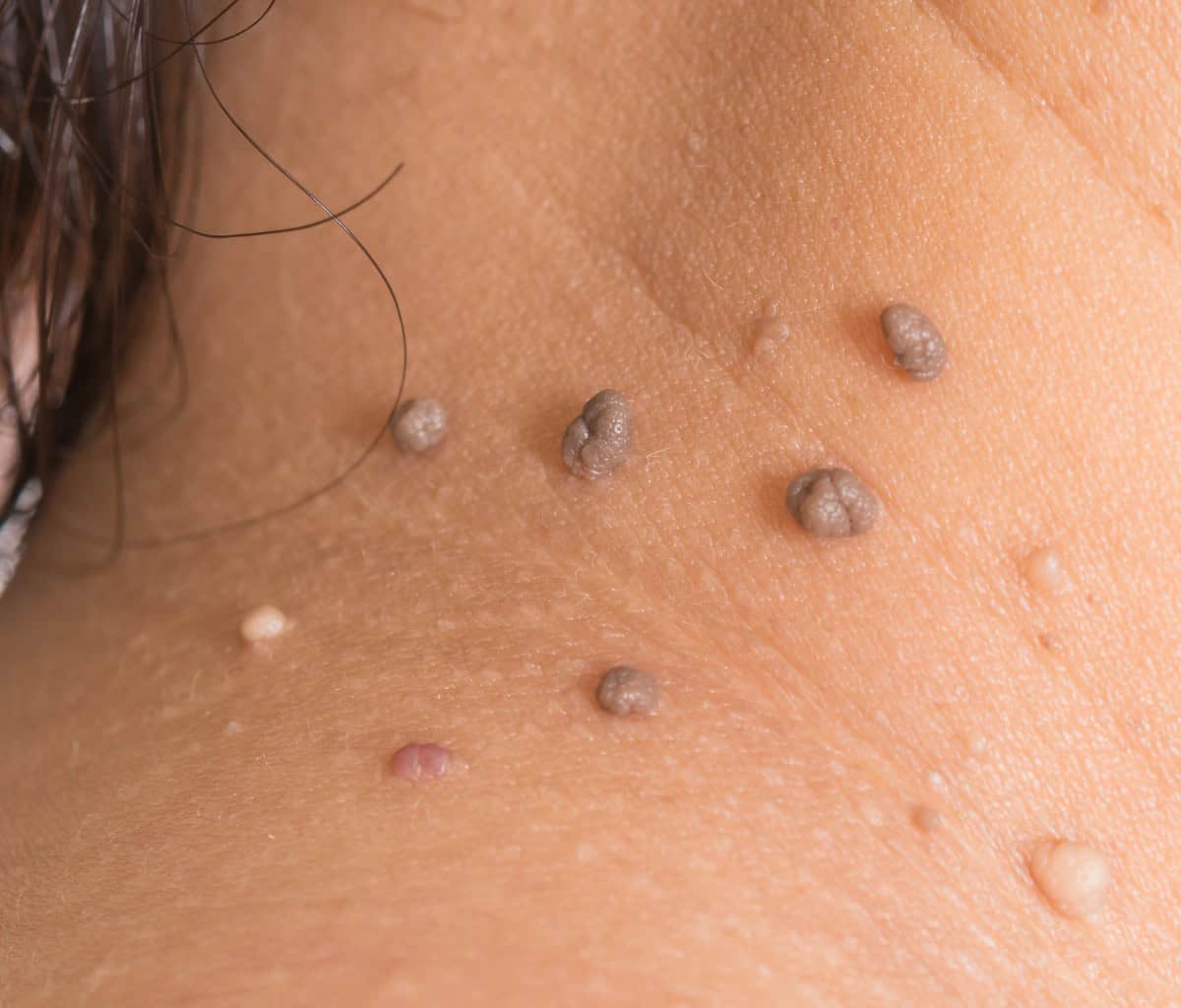
Mole Removal Healing Stages: What to Expect
One of the most searched terms (trust us at Moles.org, we know): “mole removal healing stages” and “early stage mole removal healing pictures.”
While we can’t show pictures (you’ll want to Google that separately), here’s exactly what to expect:
Surgical Excision Healing Timeline:
Immediately after (Day 0):
- Stitched wound with bandage
- Mild to moderate pain
- Some swelling and redness
- Possible minor bleeding through bandage
Days 1-3:
- Most painful period
- Swelling peaks
- Bruising may appear
- Keep dry and covered
Days 4-7:
- Pain subsiding
- Swelling decreasing
- Wound starting to heal
- Can usually get area wet (check with doctor)
Days 7-14:
- Stitches removed (timing varies by location)
- Scar is pink/red
- May feel tight or itchy
- Minimal pain
Weeks 2-6:
- Scar softening
- Color fading from red to pink
- Normal activities resumed
- Use sunscreen religiously on scar
Months 2-12:
- Scar continues maturing
- Fades from pink to lighter color
- Final appearance visible around 6-12 months
Shave Removal Healing Timeline:
- Days 1-2: Raw wound, keeps weeping
- Days 3-5: Scab forms
- Days 7-10: Scab falls off naturally (don’t pick!)
- Weeks 2-4: Pink skin underneath healing
- Months 1-3: Color normalizing
Laser Removal Healing Timeline:
- Immediately: Raw, red area
- Days 1-3: Darkening of treated area
- Days 4-7: Scab/crust formation
- Days 7-14: Scab falls off
- Weeks 2-8: Healing, may need additional sessions
Signs of Normal Healing:
- Gradual reduction in redness
- Decreasing pain
- Itching (sign of healing)
- Pink/red scar initially
- Some tightness around wound
When to Call Your Doctor:
- Increasing pain after first few days
- Red streaks extending from wound
- Pus or yellow/green discharge
- Fever
- Excessive bleeding
- Wound opens up
- Severe swelling
- Foul odor from wound
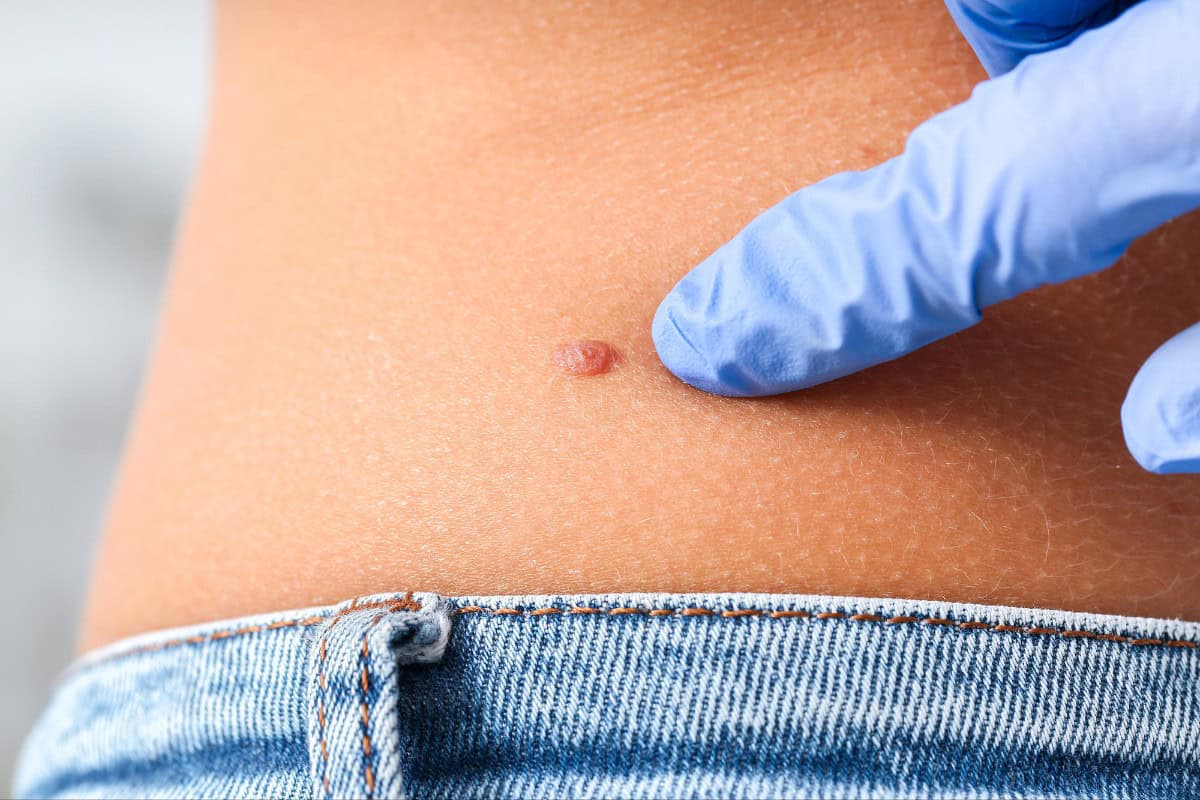
Mole Removal Scars: The Honest Truth
“Does mole removal leave a scar?” The question everyone asks but fears the answer to.
The truth from the experts at Moles.org: Usually yes, but it depends on the method and your skin’s healing ability.
Scarring by Method:
Surgical Excision:
- Always leaves a linear scar
- Size depends on mole size (usually 2-3x mole diameter)
- Usually fades to thin line
- Most predictable scarring
- Proper suturing technique minimizes scar
Shave Removal:
- Usually minimal scarring
- May leave slight indentation or texture change
- Less noticeable than surgical scar typically
- Risk of hypertrophic (raised) scar
Laser Removal:
- Minimal scarring when done correctly
- Risk of hypopigmentation (light spots)
- May have texture changes
- Results vary widely based on practitioner skill
Cryotherapy:
- High risk of permanent light spots
- Especially problematic for dark skin
- May have texture changes
- Often leaves noticeable mark
Factors Affecting Scarring:
- Location: Face heals better than back/shoulders
- Age: Younger skin heals with less scarring
- Skin type: Darker skin more prone to hyper/hypopigmentation
- Genetics: Some people scar more easily (keloid tendency)
- Aftercare: Proper care dramatically affects outcome
- Sun exposure: UV damage worsens scars
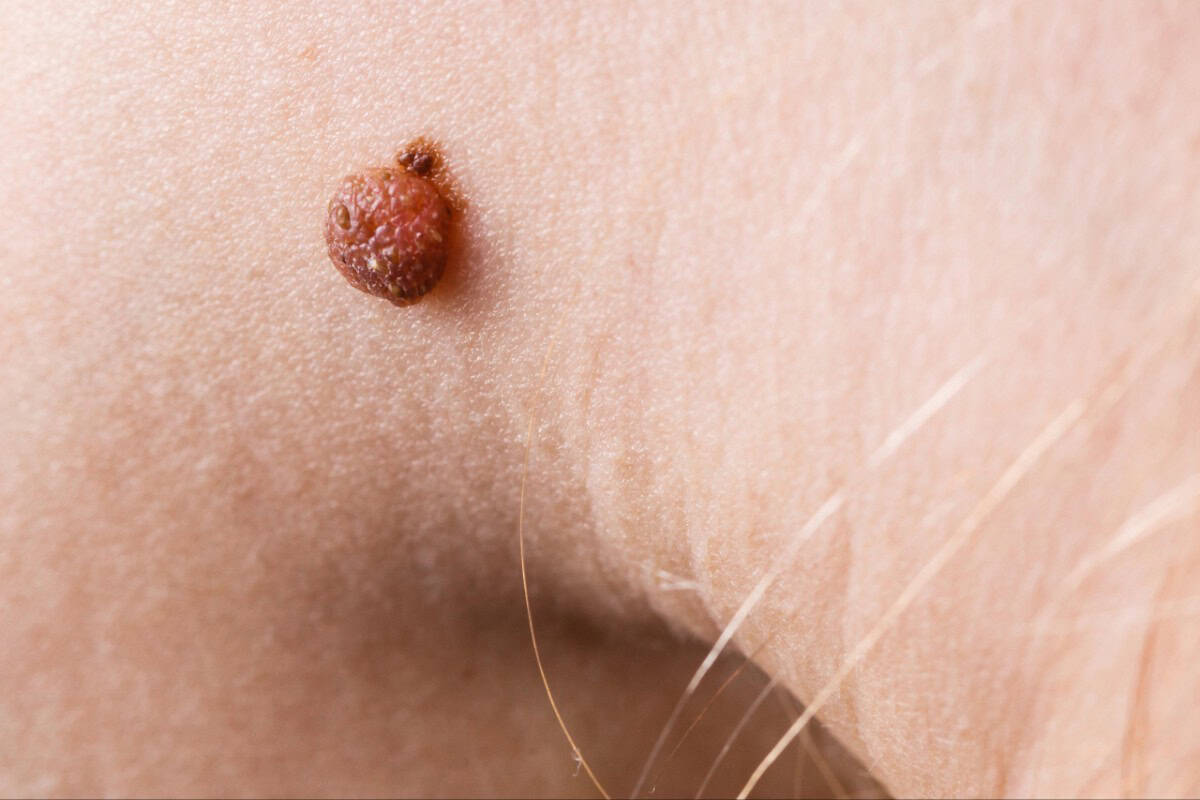
Minimizing Scars: Your Post-Removal Battle Plan
At Moles.org, we’ve seen every scar story imaginable. Here’s how to give yourself the best shot at minimal scarring:
The First 48 Hours (Critical Window):
- Keep it covered and moist (your wound is not jerky)
- No touching with dirty fingers (we’re looking at you, fidgeters)
- Follow your doctor’s instructions like they’re worth a million bucks (they kind of are)
- Ice if swollen (but don’t freeze your face off)
Week 1-2 (The Healing Phase):
- Vaseline or recommended ointment 2-3x daily
- Keep covered until scab forms
- No picking at scabs (seriously, NO PICKING)
- Avoid strenuous exercise that makes you sweat
- Sleep with your head elevated if it’s a facial mole
Weeks 2-6 (The Patience Test):
- Gentle washing once scab falls off naturally
- Start scar treatments if recommended
- Massage gently to flatten scar (after full healing)
- Protect from sun religiously with SPF 50+
Long-Term Scar Management:
- Silicone sheets or gel (clinically proven to help)
- Vitamin E oil (jury’s still out, but can’t hurt)
- Laser scar revision if needed
- Microneedling for texture improvement
- Time (your best friend—most scars improve dramatically over 6-12 months)
Red Flags During Healing:
Call your doctor if you notice:
- Increasing redness, warmth, or swelling after day 3
- Pus or yellow/green discharge
- Red streaks extending from wound
- Fever above 100.4°F
- Pain that gets worse instead of better
- Wound separation or opening
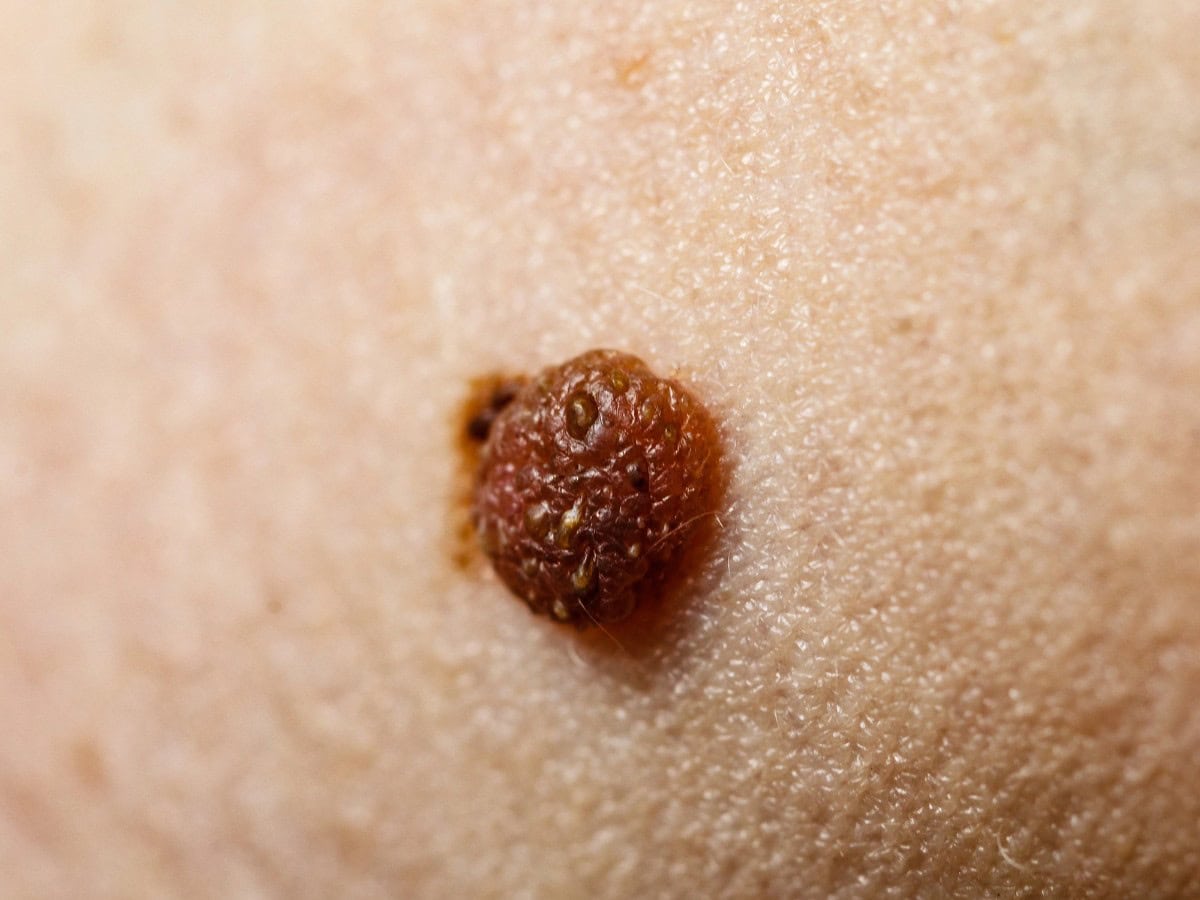
DIY Mole Removal: Just Don’t (But Here’s Why People Try)
Look, we’re called Moles.org, not MolesGoWrongProfessionally.org, so we have to address the elephant in the room: at-home mole removal.
The Tempting Online “Solutions” People Try:
Apple Cider Vinegar Method:
- The promise: Acid burns mole away
- The reality: Acid burns everything away
- Infection risk: High
- Scarring risk: Almost certain
- Cancer detection: Impossible
- Moles.org rating: 0/10, would not recommend
“Mole Removal Pens”:
- The promise: Professional results at home
- The reality: Glorified burning device
- Infection risk: Moderate to high
- Scarring risk: High
- Cancer screening: None
- Price: $20-$100 (plus the cost of fixing what you damaged)
“Natural” Mole Removal Creams:
- The promise: Herbal magic
- The reality: Sketchy chemicals with no FDA oversight
- Often contain bloodroot (escharotic—tissue-destroying)
- Can cause deep, disfiguring scars
- Cancer cells left behind: Very possible
Cutting/Shaving at Home:
- We shouldn’t even have to say this
- Massive infection risk
- Severe bleeding possible
- Incomplete removal guaranteed
- Nerve damage potential
- Moles.org official statement: ABSOLUTELY NOT
Freezing Kits (Like for warts):
- Not cold enough for moles
- Uneven application
- Damage to surrounding skin
- Rarely effective
- Just… don’t
Why DIY Mole Removal Is Playing Russian Roulette
The Cancer Issue:
That mole you’re burning off with vinegar? It could be melanoma. By destroying it at home, you’re:
- Eliminating the ability to biopsy it
- Potentially allowing cancer to spread undetected
- Creating scar tissue that masks future cancer signs
- Literally gambling with your life to save $200
The Infection Issue:
Your bathroom is not sterile. Your tools are not sterile. Your hands are not sterile. Infections from DIY removal can lead to:
- Cellulitis (spreading skin infection)
- Abscess formation
- Sepsis (life-threatening blood infection)
- Permanent scarring worse than any mole
- Hospital stays that cost WAY more than professional removal
The Scarring Issue:
Professional mole removal is an art. DIY removal is… not. You risk:
- Keloid scars (raised, thick scars)
- Hypopigmentation (permanent white spots)
- Crater-like depressions
- Hypertrophic (lumpy) scars
- Scars that are WAY more noticeable than the mole ever was
Real Stories from Moles.org’s “Don’t Try This at Home” Files:
Sarah’s Apple Cider Vinegar Adventure:
- Tried removing facial mole with ACV
- Ended up with third-degree burn
- Required skin graft
- Now has 2-inch scar instead of 3mm mole
- Total cost: $15,000+ medical bills
Mike’s Mole Pen Mishap:
- Bought pen online for $50
- “Removed” mole on back
- Actually was dysplastic nevus (pre-cancerous)
- Returned a year later as melanoma
- Now undergoing chemotherapy
The Only “At-Home” Mole Management That’s Safe
Mole Monitoring (Not Removal):
- Take monthly photos of suspicious moles
- Use the ABCDEs guide
- Document any changes
- Show photos to dermatologist
- This is smart self-care
Over-the-Counter Treatments to AVOID:
- Anything promising to “remove” moles
- “Mole erasers”
- “Natural mole vanishers”
- Basically anything on late-night TV
When Someone Suggests DIY Removal:
Just show them this guide from Moles.org. We’ve literally made it our mission to educate people about moles. Trust the people who named their whole organization after these little skin bumps.
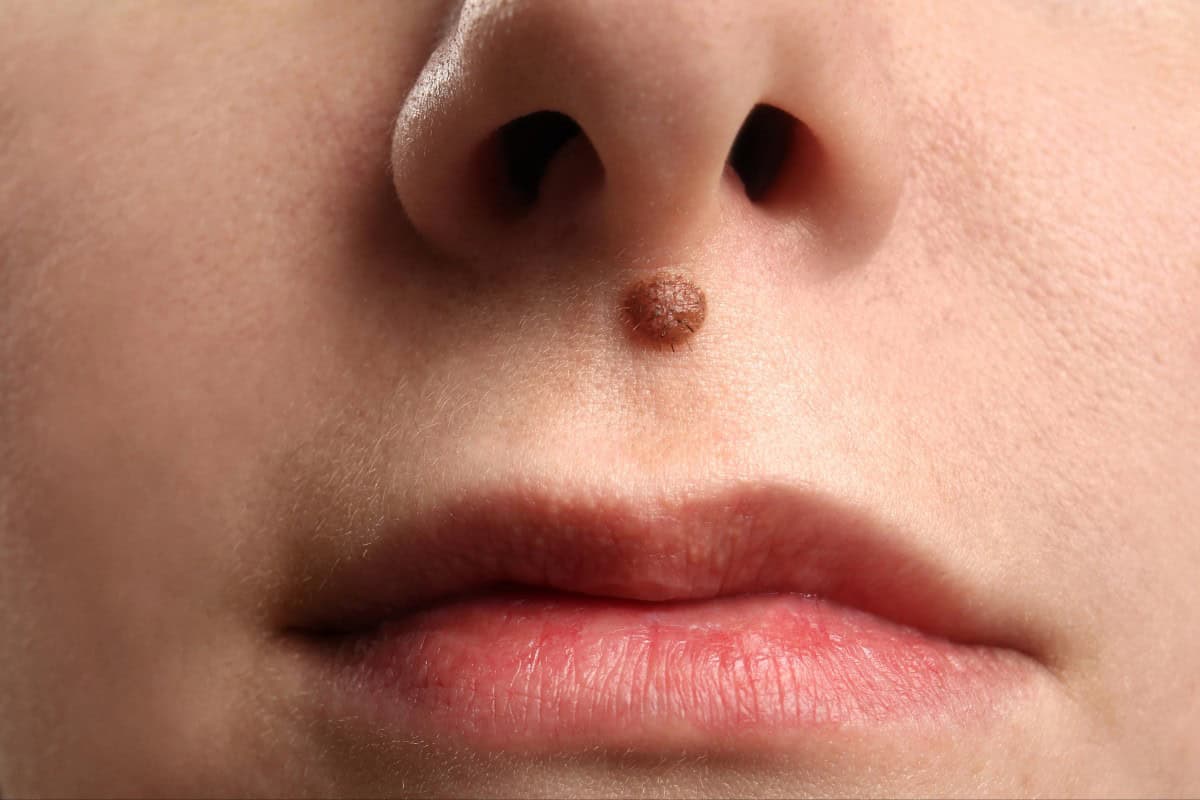
Mole Removal for Special Cases
Facial Moles: High-Stakes Removal
Your face is not the place to cut corners (pun intended). Special considerations:
Best Methods for Facial Moles:
- Shave excision for raised moles
- Surgical excision for suspicious moles
- Laser for very small, flat moles
- Always see a specialist for face
Plastic Surgeon vs. Dermatologist:
- Dermatologist: Cancer screening expertise, good surgical skills
- Plastic surgeon: Superior cosmetic outcomes, less cancer training
- Ideal: Dermatologist for diagnosis, plastic surgeon for removal if benign and cosmetic
Facial Scar Minimization:
- Request plastic closure techniques
- Ask about running scar along natural skin lines
- Consider staged approach for large moles
- Invest in professional scar care
Moles on the Scalp: The Hidden Challenge
Scalp moles are tricky because:
- Hair makes monitoring difficult
- Constantly irritated by brushing/combing
- Higher melanoma risk if repeatedly traumatized
- Require special closure techniques
Scalp-Specific Concerns:
- Will hair grow back? Usually yes, if follicles not damaged
- Healing time: Longer than other areas
- Bleeding: More profuse due to rich blood supply
- Suture removal: Need someone else to help
Eyelid Moles: Proceed with Extreme Caution
This is ophthalmologist or oculoplastic surgeon territory.
Why Eyelid Moles Are Special:
- Proximity to eye
- Thin, delicate skin
- Functional importance of eyelid
- Higher complication risk
Never DIY or Use Laser on Eyelid Moles:
- Risk of eye damage
- Risk of eyelid malformation
- Risk of vision loss
- Always needs surgical specialist
Moles in “Personal” Areas
Yes, you can get moles removed from… everywhere. Including there.
Genital/Anal Area Moles:
- Require same cancer screening as elsewhere
- Often removed for comfort (friction)
- Healing takes longer
- Keep area clean and dry
- No embarrassment necessary—doctors have seen it all
Congenital Giant Moles: The Big Kahuna
Large moles present at birth (>8 inches) are a special category:
Unique Risks:
- 5-10% lifetime risk of melanoma
- Often requires multiple staged surgeries
- May involve tissue expansion
- Plastic surgery often necessary
- Best addressed in childhood
Treatment Approaches:
- Serial excisions over time
- Skin grafting
- Tissue expansion techniques
- Laser treatment for surface areas
- Close surveillance if not removed
Mole Removal Recovery: What to Really Expect
The timeline nobody tells you about (until now, thanks to your friends at Moles.org):
Day 0-1 (Removal Day):
- Numbness wears off in 2-6 hours
- Expect throbbing/aching pain (usually mild)
- Bruising and swelling begin
- Bandage gets bloody (this is normal)
- Take it easy (yes, even from that small mole)
Days 2-7:
- Pain peaks around day 2, then improves
- Swelling and bruising maximal around day 3
- Itching begins (sign of healing)
- Keep wound covered and moist
- No gym, swimming, or hot tubs
Week 2:
- Sutures removed (if used)
- Scab forming or formed
- Scar looks its worst (don’t panic)
- Can resume light activity
- Still avoid swimming
Weeks 3-6:
- Scab falls off naturally
- Scar appears red and raised
- Gentle massage helps
- Can resume all activities
- Start scar treatments if recommended
Months 2-6:
- Scar begins fading
- Redness decreases
- Texture smooths
- Still protect from sun
6-12 Months:
- Scar reaches final appearance
- Most improvement happens here
- May be nearly invisible or slightly visible
- Sun protection still crucial
Activity Restrictions by Area:
Face:
- No strenuous exercise: 3-5 days
- No makeup: 5-7 days
- No swimming: 2 weeks
Trunk/Extremities:
- No heavy lifting: 7-14 days
- No running/cardio: 7-10 days
- No swimming: 2-3 weeks
Back/Shoulders:
- Longest healing time
- No heavy lifting: 3-4 weeks
- Highest tension on wound
When Moles Come Back: The Unwanted Sequel
“I had it removed! Why is it back?!”
Don’t panic. Here’s what’s happening:
Recurrent Moles (Non-Cancerous):
Why Moles Recur:
- Incomplete removal (especially with shave method)
- Mole cells left at wound edges
- Deep component not reached
- Scar tissue that looks like mole
Recurrence Rates by Method:
- Shave removal: 20-30%
- Surgical excision: <5%
- Laser: 10-40% (varies widely)
What Recurrent Moles Look Like:
- Often darker than original
- May be partially removed
- Can have irregular color (mix of scar and mole)
- Usually appear within 6-12 months
When to Worry About Recurrence:
Actually, this is important: Recurrent moles need biopsy.
Why? Because:
- Scar tissue can mask melanoma
- Healing changes can look like dysplasia
- Better safe than sorry
- Your dermatologist needs to know
Treating Recurrent Moles:
- Full surgical excision (deeper this time)
- Don’t try shave method again
- Consider going wider
- Send for pathology again
The Mole Removal Consultation: What to Ask
Don’t leave your doctor’s office without answers. Here’s your Moles.org-approved question list:
Before the Procedure:
About Your Specific Mole:
- Do you recommend removing this mole? Why or why not?
- Is there any chance this could be cancerous?
- What method do you recommend for my specific mole?
- What will the scar likely look like?
- How long is the recovery?
About the Procedure:
- Where will this be performed? (office vs. surgical center)
- What type of anesthesia will be used?
- How long will the procedure take?
- Will you send it for pathology testing?
- What’s your experience with this type of removal?
About Costs:
- What’s the total out-of-pocket cost?
- Is this covered by my insurance?
- Do I need pre-authorization?
- Are there additional costs? (pathology, facility fees, etc.)
About Recovery:
- When can I return to work/exercise/activities?
- What are the potential complications?
- What should I do if I have problems?
- When will sutures be removed?
- What restrictions will I have?
About Results:
- When will I know the pathology results?
- What’s the chance this mole will come back?
- Will I need follow-up appointments?
- What scar treatment do you recommend?
Red Flags: When to Run from a Mole Removal Provider
Not all mole removers are created equal. Here’s when Moles.org says “NOPE”:
Run If They:
- Offer to remove moles without examining them first
- Don’t plan to send ANY moles for pathology
- Promise “scar-free” removal (nothing is truly scar-free)
- Use laser on suspicious moles (big no-no)
- Pressure you to remove moles you’re not concerned about
- Are not board-certified (dermatology or plastic surgery)
- Offer “group deals” on mole removal (it’s not Groupon material)
- Can’t answer questions about their training
- Don’t discuss risks and complications
- Make it seem overly simple or casual
Good Signs:
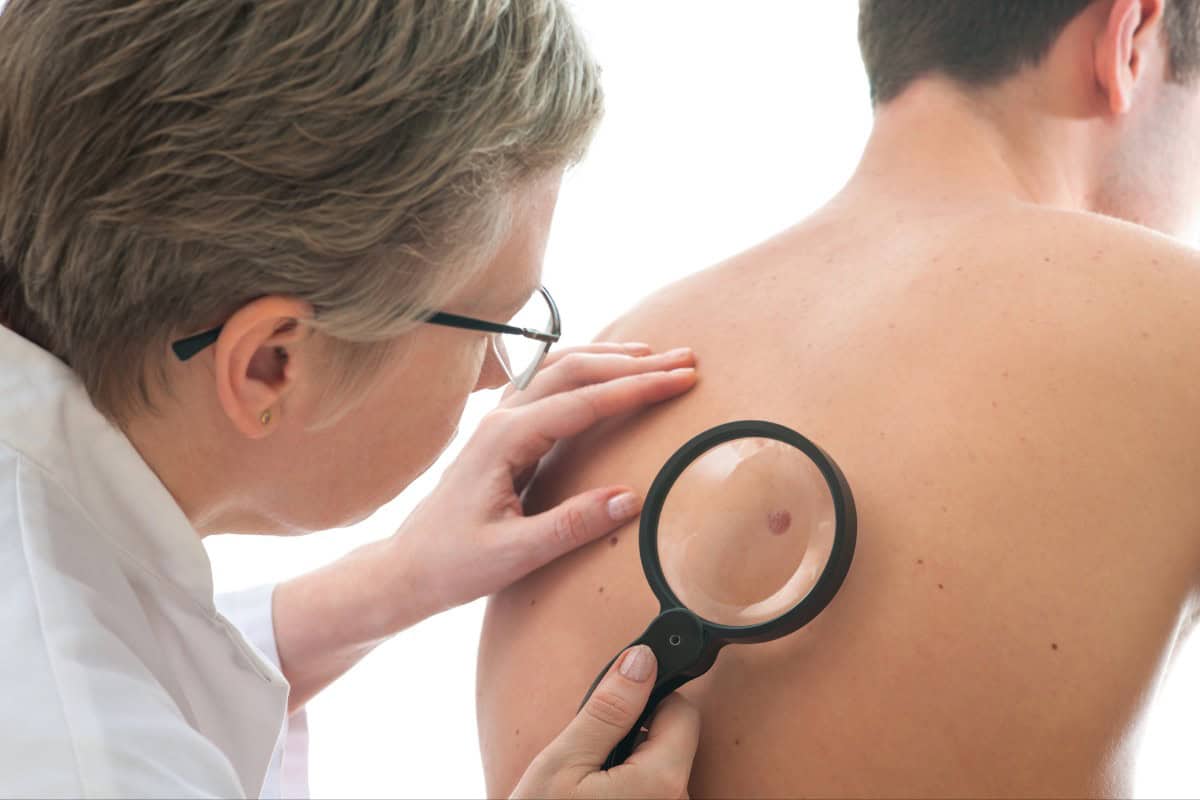
- Thorough examination with dermatoscope
- Discussion of cancer concerns
- Clear explanation of scar expectations
- Honest about what can/cannot be done
- Board certification displayed
- Before/after photos of their work
- Clear cost breakdown
- Detailed aftercare instructions
- Follow-up plan included
Special Populations: Kids, Pregnancy, and Seniors
Mole Removal in Children:
When to Consider Removal in Kids:
- Congenital moles with cancer risk
- Moles causing physical problems
- Rapidly changing moles
- Psychological distress from cosmetic concerns
Special Considerations:
- Require general anesthesia (usually under age 10)
- Higher cost due to anesthesia
- May need pediatric dermatologist
- Consider waiting if purely cosmetic
- Kids heal remarkably well
Mole Removal During Pregnancy:
The Short Answer: Wait if you can.
Why:
- Pregnancy causes mole changes (hormones)
- Anesthetics cross placenta
- Healing may be different
- Hard to distinguish normal pregnancy changes from concerning changes
When Removal Can’t Wait:
- Suspicious for melanoma
- Rapidly changing
- Bleeding/problematic
Safe Anesthetics in Pregnancy:
- Local lidocaine without epinephrine: Category B (generally safe)
- Keep dose low
- Second trimester is safest time
Mole Removal in Seniors:
Special Considerations:
- Healing slower
- Higher complication risk
- More likely on blood thinners
- Skin more fragile
Benefits for Seniors:
- More time for suspicious moles to show their colors
- Can often identify truly concerning moles
- Lifetime sun damage makes monitoring crucial
- Don’t skip removal due to age—melanoma doesn’t care how old you are
Mole Removal Technology: What’s New and What Works
Emerging Technologies:
Radiofrequency Devices:
- Ellman Surgitron and similar
- Causes less thermal damage than traditional electrocautery
- Faster healing
- Less scarring than older methods
- Good for small cosmetic moles
Plasma Pen Technology:
- Uses ionized gas instead of cutting
- Minimal bleeding
- Less surrounding tissue damage
- Jury still out on long-term scarring
- Not suitable for deep or suspicious moles
Advanced Laser Systems:
- Erbium lasers for superficial moles
- CO2 lasers for raised moles
- Still can’t biopsy what’s been lasered
- Best for tiny, clearly benign moles
3D Imaging and AI:
- Helps monitor moles over time
- Can detect subtle changes
- Not a replacement for expert examination
- Great for tracking multiple moles
What’s Hype vs. What’s Hope:
- Hype: “Scar-free laser removal”
- Hope: Better scar outcomes with new techniques
- Hype: “Natural mole erasers”
- Hope: Better understanding of mole biology
- Hype: AI replacing dermatologists
- Hope: AI assisting dermatologists
The Bottom Line from Moles.org
We’ve covered everything from the scientific to the silly, from the serious to the scarring. Here’s what the mole experts want you to remember:
The Golden Rules:
- When in doubt, check it out – See a dermatologist for changing moles
- Biopsy beats regret – Always send suspicious moles for testing
- Method matters – Choose the right technique for your mole
- Scars happen – But proper care minimizes them
- DIY = DON’T – Seriously, just don’t
- Insurance is weird – But medical necessity usually wins
- Healing takes time – Give scars 6-12 months to mature
- Not all providers are equal – Board certification matters
- Ask questions – It’s your skin and your money
- Sun protection is forever – Especially on scars
Your Mole Removal Action Plan:
Step 1: Self-Examine
- Use the ABCDE guide
- Take photos of concerning moles
- Note any changes
Step 2: See an Expert
- Ideally a board-certified dermatologist
- Get a full body check
- Discuss concerns openly
Step 3: Make Informed Decisions
- Understand why removal is recommended
- Ask about all options
- Consider the trade-off: mole vs. scar
Step 4: Choose the Right Method
- Match method to your situation
- Consider location and mole type
- Understand risks and benefits
Step 5: Prepare for Procedure
- Follow pre-op instructions
- Arrange for help if needed
- Take photos before removal
Step 6: Nail the Aftercare
- Follow instructions religiously
- Keep wound moist and covered
- Protect from sun
- Be patient with healing
Step 7: Monitor Results
- Attend follow-up appointments
- Watch for recurrence
- Treat scars appropriately
- Continue skin surveillance
Final Thoughts from Your Mole Mavens
At Moles.org, we’ve seen it all: the good, the bad, and the “why did you try to remove that with apple cider vinegar?!” Our mission is simple—help you make informed decisions about those little (or not so little) brown spots that dot your landscape.
Remember: Moles are incredibly common. Most are harmless. Many can be safely removed. But the key is doing it right—with proper medical guidance, appropriate methods, and realistic expectations.
Your skin is the largest organ you’ve got. It’s also the one everyone sees. Treat it with respect, give it the professional attention it deserves, and for the love of all things dermatologic, don’t try to burn moles off with household products.
Stay safe, stay informed, and keep those skin checks regular!
— The Mole Experts at Moles.org (We really, really love talking about moles.)
P.S. If your mole looks weird, don’t Google it for three hours at 2 AM. Just call a dermatologist. Trust us on this one. We’re the mole people.